If you are seriously concerned about scarring, consider discussing the following methods of scar minimization and prevention with your surgeon. Your surgeon may be able to prescribe additional treatments that lower your chances of scarring.
Risk Factors For Scarring
As we age, our skin becomes less elastic and becomes thinner. This is because collagen (which makes the skin elastic) changes as we age, and the fat layer under our skin becomes thinner. The result of these changes, along with sun exposure, smoking, exposure to the environment and other lifestyle issues, means that skin does not heal as well or as quickly as we age. The benefit to age is that the imperfections that occur over time, like sun damage, work to help conceal scars that might be more obvious on younger skin.
Some skin colorations are more likely to scar than others. Those with dark skin tones are more likely to form hypertrophic and keloid scars, which are characterized by an overgrowth of scar tissue. However, some scars tend to blend in better with darker skin while people with fairer skin may find that their scars are more noticeable.
A large incision is much more likely to leave a scar than a small incision. The deeper and longer the incision, the longer the healing process will take and the greater the opportunity for scarring. A larger incision may be exposed to more stress as you move, which can cause slower healing.
You may be one of the genetically blessed people who seem to heal magically, quickly and easily with minimal scarring, or you may be diabetic and your skin tends to heal slowly. How quickly you heal is a personal thing and can change with illness or injury.
Smoking
Not only does smoking increase your risk for scars, it can also slow your healing. Smoking is such a significant risk factor that many plastic surgeons will not operate on a patient if he does not quit smoking COMPLETELY for at least 2 weeks prior to surgery.
Drinking
Alcohol dehydrates both the body and skin, which decreases your overall state of health. While your wound is healing, avoid alcohol and focus on non-caffeinated beverages.
Nutrition
Eat a balanced diet with an emphasis on protein intake. Protein makes up the building blocks of healing skin, so it is essential to provide your body with adequate protein (chicken, pork, fish, seafood, beef, dairy products) to allow your skin to heal. If you do not like eating meat, soy products provide an excellent alternative as a lean protein source.
Hydration
Dehydration happens when you are not taking in enough fluids. In severe cases, this can cause electrolyte imbalances and heart issues. In less severe cases, you will feel thirsty and your overall health will be diminished. Staying well hydrated (Tip: If you are well-hydrated, your urine will be almost colorless or light in color) will help keep your healing headed in the right direction.
Your Weight
If you are overweight, you may be at greater risk for scarring. Why? The fat under your skin can work against your surgeons best efforts to close your incision seamlessly.
Rest
If your doctor suggests that you rest for two weeks, don’t go back to work after one week of healing. Exhausting yourself will not help your wound heal and can actually slow healing.
Proper Wound Care
Taking the steps recommended by your surgeon may be the single most important thing you can do to prevent scars. Taking measures to prevent infection, refraining from using ointments and remedies that are not prescribed, and other general incision care techniques are essential to healing without scars.
Identify Infection Quickly
If your incision becomes infected, it is important that you can identify the signs of infection and seek help from your physician immediately. An infection can seriously impair healing and can contribute to scarring.
Chronic Illness
Diabetes and many other illnesses can slow healing. For the best possible outcome, your illness should be as well-controlled as possible before surgery and during your recovery. For example, for a diabetic it is essential for blood glucose levels to be within normal limits as much as possible as high levels slow healing.
Stress on Your Incision
Putting stress on your incision by lifting, bending or doing anything that stretches or puts tension on the incision should be avoided. This stress can pull the incision apart, delaying healing and often making the wound larger than it needs to be, which increases the size of your scar.
Exposure to Sunlight
Avoid having the sun on your incision whenever possible. If your scar is in place that is difficult to cover, such as your face, invest in a good sunscreen. Your surgeon can tell you when it is safe to apply ointments, but it is usually safe to do so when the sutures are removed or the incision has closed completely.
Wound Care Treatment
Silicone Wound Treatments:
Silicone wound dressings and Silicone gels are best for after surgery scar care. Studies have shown that silicone can help reduce scarring and is commonly used after plastic surgery. Discuss Silicone dressings Silicone gels with your surgeon. Dr. Hochstein highly recommends the Bio Corenum for after surgery on the incisions. Bio Corenum is the only FDA approved Scar Gel on the Market today and can only be found at Dr. offices.
Incision Placement:
In some surgeries, the placement of the incision is not absolute. You may be able to talk to your surgeon about where the incision is placed to either hide or help minimize scars. For example, Face Lift/Neck lift incisions are placed behind and inside the ear when possible, tummy tuck incisions may be disguised by a bikini.
Steroid Injections:
If you are prone to forming keloid scars, talk to your surgeon about having a steroid injection to prevent the formation of another keloid.
 Model
Model
Minimizing Scars After Surgery
Benifits
- Painless, comfortable procedure
- Customizable treatment
- Amazing, ablative results
- Little to no downtime

Halo™ Hybrid Fractional Laser Halo™ is the world’s first hybrid laser that features two laser wavelengths, one ablative and one-non-ablative, to significantly improve the appearance of scars. This treatment is ideal for patients with mild acne scarring or hypertrophic (raised) scars, especially those that are a result of surgical incisions. Each laser wavelength can be adjusted to target the ideal skin depth and microscopic treatment zone(s), which allows for a completely customized procedure to meet each patient’s specific needs. Halo™ also has integrated cooling that keeps the skin cool and patients comfortable throughout the entire procedure. Patients will see a noticeable improvement after just one treatment, but the recommended series of three treatments at six-week intervals may be needed to achieve optimum results.
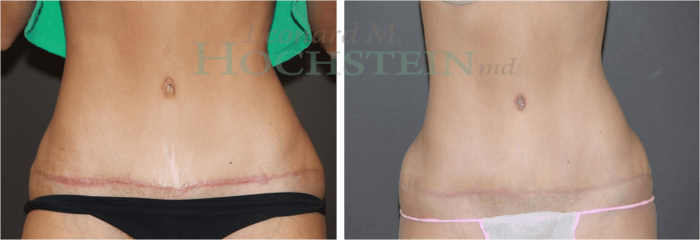
Dr. Hochstein’s Scar Management Program

Bio-Corneum
Our chosen product to address scarring is Bio-Corneum+ (or BC+). Using BC+ will provide the best environment for the scar to heal and will help speed up the healing process. We recommend that all of our patients use this after their sutures are removed and their wound is closed. We carry this in our office as a convenience for you. It is a self-adhering, self-drying silicone gel that also contains a mild broad spectrum SPF 30. At suture removal, start applying BC+ twice a day to your scar for at least twelve weeks, or until you stop seeing noticeable results. If you have a tendency to form hypertrophic or keloid scars, you may want to use it for 6 months to a year. BC+ has been shown to help prevent the formation of these types Scar of scars. One drop is enough to cover a three inch scar. Spread a very thin layer of BC+ over the scar area. It should dry within a few minutes and will form a slick surface over your scar. BC+ will gradually wear off throughout the day, which is why we have you reapply it at night to make sure you are getting a solid 24 hour per day exposure to the silicone. If you have any questions, please call the office.

Skin Medica TNS Ceramide Treatment Cream
Nourish and refresh the skin’s appearance after cosmetic or dermatological procedures such as:
- Dermabrasion or Microdermabrasion
- Chemical Peels
- Laser or Light Treatments
- Cosmetic Surgery Following Complete Wound Healing
Skin Medica TNS Ceramide Treatment Cream can help:
- Nourish and Refresh Aged Skin by Encouraging Rejuvenation
- Nourish an Restore the Skin’s Appearance as a Result of Environmental Exposure
- Nourish and Restore the Skin’s Appearance as a Result of Occupational Exposure
- Nourish Stressed Skin Compromised by Other Skin Conditions
Signs and Symptoms of an Infection
General Signs and Symptoms of Infection
Malaise: One of the most common symptoms of a systemic infection, or an infection that is moving through your body, is that you will feel tired and lacking in energy. You may sleep more than usual, or not feel up to doing your normal activities. These feelings are also common for patients who are recovering from surgery who do not have an infection. The difference is that when recovering from surgery most people feel a bit better each day, rather than feeling better for a few days then suddenly feeling exhausted and lethargic as can happen with infection.
Fever: A fever is often accompanied by feeling chilled. A fever can also decrease your appetite, lead to dehydration and a headache. A low-grade fever (100 F or less) is common in the days following surgery, a fever of 101 or more should be reported to the surgeon.
Signs and Symptoms of An Infected Surgical Incision
Hot Incision: An infected incision may feel hot to the touch. This happens as the body sends infection fighting blood cells to the site of infection.
Swelling/Hardening of the Incision: An infected incision may begin to harden as the tissue underneath are inflamed. The incision itself may begin to appear swollen or puffy as well.
Redness: An incision that gets red, or has red streaks radiating from it to the surrounding skin may be infected. Some redness is normal at the incision site, but it should decrease over time, rather than becoming more red as the incision heals.
Drainage From the Incision: Foul-smelling drainage or pus may begin to appear on an infected incision. It can range in color from blood-tinged to green, white or yellow. The drainage from an infected wound may also be thick, and in rare cases, chunky.
Pain: Your pain should slowly and steadily diminish as you heal. If your pain level at the surgery site increases for no apparent reason, you may be developing an infection in the wound. It is normal for increased pain if you “overdo it” with activity or you decrease your pain medication, but a significant and unexplained increase in pain should be discussed with your surgeon.